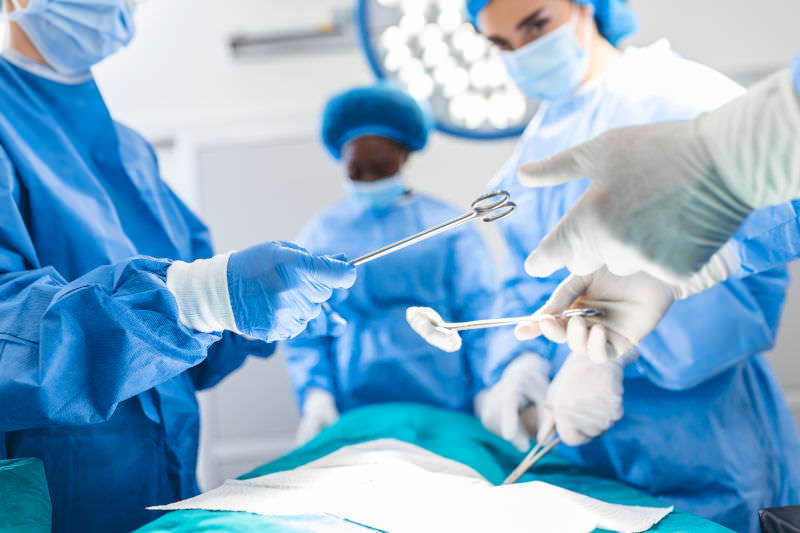
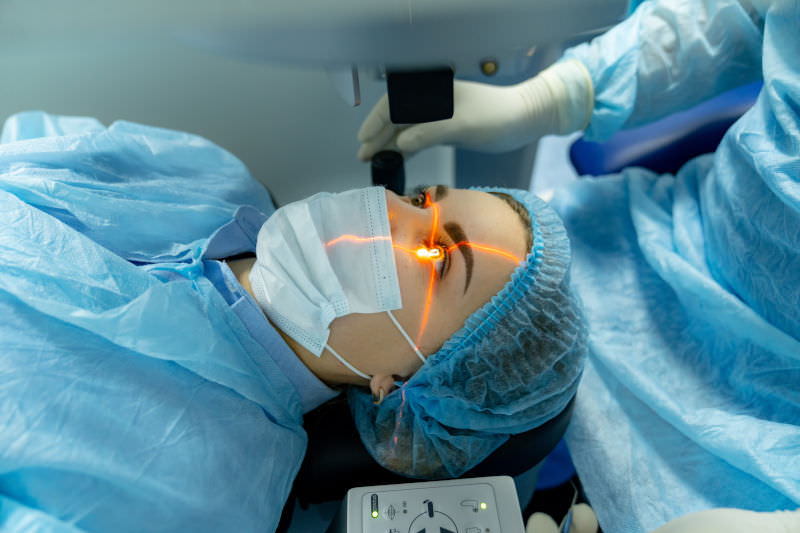
Should cosmetic firms assess their customers’ mental health?
People undergo cosmetic procedures – such as Botox, skin peels and lip fillers – for many different reasons. However, a common theme is a person’s desire to feel better about themselves and their appearance. These are concepts which are closely tied to someone’s mental wellbeing and self-image.
The National Medical Director of NHS England, Professor Stephen Powis, has called for tighter controls on private firms which carry out cosmetic procedures, particularly in relation to the mental health state of their patients prior to treatment. He believes such firms should be registered and that staff should be trained to identify mental health issues such as body-image problems.
Professor Powis stated that there were too many cosmetic firms “operating as a law unto themselves” and “the bombardment of idealised images and availability of quick-fix procedures is helping fuel a mental-health and anxiety epidemic. … We need all parts of society to show a duty of care and take action to prevent avoidable harm.”

And these are potential consequences even if the procedure goes well. If something goes wrong or harm is caused through a cosmetic procedure, it can undo this very purpose and cause severe effects.
Broadly speaking, firms carrying out cosmetic procedures owe a legal duty of care to their patients. Namely that if their standards of treatment or care fall short of the required levels, they will be liable for the injuries and harm which their negligent conduct has caused. However, one interpretation of Professor Powis’s argument is that it advocates extending that duty, in some form, to explicitly cover procedures carried out on a customer who was already suffering from mental health issues related to their self-image. Perhaps attaching liability to the firm even if the procedure was technically successful.
Psychological harm is a recognised element of many personal injury claims and may be particularly prevalent following botched cosmetic procedures. If you have undergone a cosmetic procedure or surgery and you have suffered physical or psychological harm because of negligent treatment, you may be entitled to compensation. Establishing a claim based upon a failure to assess your mental state prior to the procedure is likely to be much more difficult outside of a strict medical setting, however.
NHS Resolution and medical negligence claims against GPs
The way in which medical negligence claims against GPs are handled, changed on the 1st April 2019. Whereas previously GPs would have to arrange their own insurance against medical negligence claims, now, for work they conduct through the NHS, they will be covered by the NHS’s own insurance.
For people unfortunate enough to be affected by alleged GP medical negligence, this will bring several benefits. NHS Resolution, the organisation which deals other claims against the NHS, will now also handle claims made against GPs for work they carried out through the NHS. This means:
- A more consistent level of insurance backing. When GPs arranged their own insurance to cover negligence claims, they would often be different levels of cover. For severe injuries, this sometimes may not have been enough to cover the compensation award.
- Dealing with one opposing party. If several GPs were involved in a negligence claim, there would often be a number of different insurance companies defending the matter – depending on where each GP had taken out their cover. This would often over-complicated communication between the parties. With NHS Resolution taking over, a claimant and their solicitors will usually have just one other party to deal with.
- Better feedback from the claim. Many people make medical negligence claims to highlight serious issues, initiate change, and avoid others from suffering the same consequences in future. Part of NHS Resolution’s remit is to support the NHS in learning from instances of negligence. As such, this feedback is much better provided through NHS Resolution than insurance companies unconnected with the NHS.
Of course, not every complaint against the NHS or a GP has to be a claim for compensation. Have a look at our blog on making a complaint to the NHS for more information on this.
Unnecessary surgery
An inquiry by North Bristol NHS Trust has found that 57 patients treated by Dr Anthony Dixon between 2007 and 2017 underwent unnecessary bowel surgery. It found that the patients were not offered other, more conservative treatment options, and instead were recommended to undergo controversial mesh implant surgery by Dr Dixon.
Dr Dixon, who has now been suspended, pioneered the technique of using the mesh implant to lift prolapsed bowels. However, it has caused many of the patients to suffer severe, life-changing side effects such as chronic pain and required patients to undergo further surgery to remove the mesh implants.
Unnecessary surgery is one way in which patients can fall victim to medical negligence. At best, an unnecessary surgical procedure will only result in the potential pain, distress and recovery time of the surgery itself and any corrective surgery required. Unfortunately, however, there will often be worse complications. Some of Dr Dixon’s patients have been left with life-changing injuries as a result of the implant, as have patients fitted with other faulty, dangerous or unsuitable implants, such as the vaginal mesh implants mentioned in our previous blog.
Blood clotting agent inquiry
A high-profile inquiry has just begun, investigating a scandal involving infected blood clotting agents.
A blood clotting agent called Factor VIII was given to patients suffering from haemophilia and other blood disorders in the 1970s and 1980s. Factor VIII was produced using donor blood, some of which was contaminated with viruses such as hepatitis and HIV. It is thought that around 5,000 people contracted these viruses after being treated with the contaminated blood clotting agents.
One of the main issues for the inquiry to resolve is the question of how much was known of the dangers Factor VIII posed to patients. Screening blood products for infection began in 1991 but heat treatment to kill viruses was introduced in the mid-1980s.
A key element of liability for medical negligence claims is the standard of care. Healthcare professionals must meet the standard of reasonable care and skill for an ordinary practitioner in their field. For example, if the dangers of Factor VIII were known, or ought to have been known, by an ordinarily skilled treating doctor at the time, then there could be grounds for liability in negligence.
The inquiry has already heard harrowing accounts of lives lost and families affected by the scandal. Many of those who have lost loved ones understandably want justice for what has happened. It is hoped that this inquiry can provide them with answers, and the beginnings of accountability for the tragedies they have suffered.
If you would like specialist legal advice regarding any of the issues explored in this article, or for guidance on beginning a medical negligence claim, please get in touch with Truth Legal to see if we can help.
Further Reading
From one of the UK’s most read legal blogs.